Premenopausal osteoporosis, though often overshadowed by its postmenopausal counterpart, is a critical concern that demands attention. In this article, we delve into the intricacies of premenopausal osteoporosis treatment, exploring various aspects from understanding the condition to effective therapeutic interventions.
Contents
What Is Premenopausal Osteoporosis? 
Premenopausal osteoporosis refers to the development of osteoporosis in women before they reach menopause. Weakening of bones characterizes osteoporosis, making them more prone to fractures and breaks. Typically, postmenopausal women associate with this condition, as hormonal changes during menopause can lead to a decrease in bone density.
However, premenopausal osteoporosis occurs in women who have not yet reached menopause. It is less common than postmenopausal osteoporosis, but it can still have significant consequences for bone health.
Causes Of Premenopausal Osteoporosis
Premenopausal osteoporosis can have various causes, and it often results from a combination of factors. Here are some common causes of premenopausal osteoporosis:
- Hormonal Imbalancesosteoporosis
Estrogen is a hormone that plays a crucial role in maintaining bone density. Before menopause, estrogen levels fluctuate during the menstrual cycle. Any disruption in hormonal balance, such as low estrogen levels, can contribute to bone loss. - Genetic Factors
A family history of osteoporosis or a genetic predisposition to low bone density can increase the risk of developing osteoporosis at a younger age. - Nutritional Deficiencies
Inadequate intake of essential nutrients for bone health, such as calcium and vitamin D, can contribute to reduced bone density. These nutrients are vital for the proper formation and maintenance of bone tissue. - Medical Conditions
Certain medical conditions can affect bone health. Examples include thyroid disorders, gastrointestinal disorders (which may impair nutrient absorption), and autoimmune diseases that impact bone metabolism. - Lifestyle Factors
- Lack of physical activity or a sedentary lifestyle can contribute to weakened bones. Weight-bearing exercises are essential for maintaining bone density.
- Smoking lowers bone mass and increases the risk of fractures. Tobacco use can affect bone health directly and indirectly through hormonal and nutritional mechanisms.
- Excessive alcohol consumption is associated with an increased risk of osteoporosis. Alcohol can interfere with the body’s ability to absorb calcium, a key mineral for bone strength.
- Eating Disorders
Conditions such as anorexia nervosa or bulimia can lead to nutritional deficiencies and hormonal imbalances, adversely affecting bone health. - Chronic Stress
Prolonged exposure to high levels of stress and cortisol, a stress hormone, may contribute to bone loss. - Medications
Certain medications, such as long-term use of corticosteroids, can have adverse effects on bone density.
Identifying and addressing these risk factors is crucial for preventing or managing premenopausal osteoporosis.
Symptoms And Detection Of Osteoporosis 
Premenopausal osteoporosis often develops without noticeable symptoms until a fracture occurs, as bone loss typically progresses silently. However, some signs and risk factors may be indicative of the condition. Additionally, early detection through screenings can help identify individuals at risk. Here are some aspects related to the symptoms and detection of premenopausal osteoporosis:
- Symptoms
- No Early Symptoms: In the early stages, premenopausal osteoporosis may not present noticeable symptoms.
- Fractures: The first sign might be a fracture, especially if it occurs with minimal trauma or force. Fractures commonly affect the spine, hip, or wrist.
- Back Pain: Compression fractures in the spine may cause back pain, height loss, or a stooped posture.
- Loss of Height: Gradual loss of height over time, often due to vertebral compression fractures.
- Change in Posture: A stooped or hunched posture, known as kyphosis, may develop due to compression fractures in the spine.
- Bone Pain: Some individuals may experience bone pain, especially if fractures have occurred.
- Detection
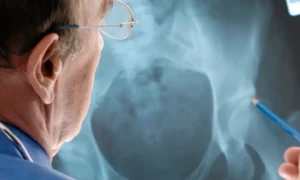
- Bone Density Testing
Dual-energy X-ray absorptiometry (DEXA or DXA) scans are commonly used to measure bone density. This non-invasive test assesses bone strength and helps in the diagnosis of osteoporosis. - Medical History and Physical Examination
Healthcare providers will inquire about personal and family medical histories, assess risk factors, and conduct a physical examination to check for signs like height loss or changes in posture. - Blood Tests
Blood tests may be conducted to measure levels of certain markers related to bone health, such as calcium, vitamin D, and hormones like estrogen.
- Bone Density Testing
- Fracture Risk Assessment
Tools like FRAX (Fracture Risk Assessment Tool) may be used to estimate an individual’s 10-year probability of experiencing a major osteoporotic fracture based on clinical risk factors. - Imaging Studies
X-rays or other imaging studies may be performed to identify existing fractures or signs of bone loss.
Premenopausal Osteoporosis Treatment Options
The treatment of premenopausal osteoporosis involves a multifaceted approach that addresses the underlying causes, promotes bone health, and reduces the risk of fractures. Treatment options may include lifestyle modifications, nutritional interventions, medications, and hormonal therapies. Here is a detailed overview of premenopausal osteoporosis treatment options:
Lifestyle Modifications
- Weight-Bearing Exercise: Regular weight-bearing exercises, such as walking, jogging, and resistance training, can help improve bone density and strength.
- Balance and Strength Training: These exercises can enhance stability and reduce the risk of falls and fractures.
Nutritional Interventions
- Calcium and Vitamin D Supplementation: Adequate calcium and vitamin D intake is crucial for bone health. Supplements may be recommended if dietary intake is insufficient.
- Healthy Diet: Consuming a balanced diet with a focus on calcium-rich foods (e.g., dairy products, leafy green vegetables) and vitamin D sources (e.g., fatty fish, fortified foods) is essential.
Medications
- Bisphosphonates: Bisphosphonates work to maintain the strength and integrity of your bones by slowing down or halting the natural processes that lead to the dissolution of bone tissue. By preventing the loss of calcium and other minerals, these medications contribute to the preservation of bone strength and structure.
- Selective Estrogen Receptor Modulators (SERMs): Medications like raloxifene can mimic the beneficial effects of estrogen on bone density without affecting other tissues.
- Teriparatide: Teriparatide is a medication for osteoporosis designed to enhance bone strength and lower the likelihood of bone fractures. Administered through a self-administered daily injection, it is typically used for a duration of up to two years. Teriparatide operates as a treatment based on parathyroid hormone.
- Denosumab: Denosumab, marketed under the name Prolia®, is a medication used to treat osteoporosis by enhancing bone strength and reducing the risk of fractures. Administered through an injection every six months, it is typically not the initial choice for osteoporosis treatment.
Hormonal Therapies
- Hormone Replacement Therapy (HRT): Estrogen replacement therapy may be considered for women with estrogen deficiency. However, the decision to use HRT should be carefully weighed, considering individual health risks and benefits.
Addressing Underlying Causes
- Management of Contributing Medical Conditions: Treating underlying medical conditions that contribute to osteoporosis, such as thyroid disorders or gastrointestinal disorders, is essential.
- Addressing Hormonal Imbalances: If hormonal imbalances are identified, such as irregular menstrual cycles, addressing these issues may be part of the treatment plan.
Regular Monitoring
- Periodic monitoring of bone density through DEXA scans can help assess the effectiveness of treatment and guide adjustments if needed.
It’s important to note that the choice of treatment depends on individual factors, including the severity of osteoporosis, overall health, and the presence of other medical conditions. Treatment plans are often tailored to the specific needs of each individual. Additionally, lifestyle modifications, including a healthy diet and regular exercise, are fundamental components of managing premenopausal osteoporosis.
Consultation with a healthcare professional is crucial for the proper evaluation and development of a personalized treatment plan based on individual circumstances and medical history.
Alternative Treatments And Therapies 
In addition to conventional medical treatments, there are alternative therapies and lifestyle approaches that may complement the management of premenopausal osteoporosis. It’s crucial to discuss these options with a healthcare professional before incorporating them into a treatment plan. Here are some alternative treatments and therapies that may be considered:
- Nutritional Supplements
- Calcium and Vitamin D: Adequate intake of calcium and vitamin D is vital for bone health. If dietary sources are insufficient, supplements may be recommended.
- Herbal Supplements
Limited scientific evidence supports the efficacy of herbs and plant-based supplements such as red clover and black cohosh, which are believed to have bone-supporting properties. Exercise caution when considering their use. - Acupuncture
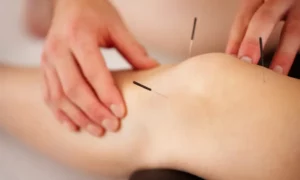
Acupuncture, an ancient Chinese practice involving the insertion of thin needles into specific points on the body, is sometimes explored for its potential benefits in managing bone health. Research on its effectiveness for osteoporosis is ongoing. - Mind-Body Techniques
Stress-reducing practices such as meditation and mindfulness may indirectly contribute to bone health by promoting overall well-being and reducing the impact of chronic stress. - Dietary Changes
A diet rich in fruits, vegetables, and whole foods provides essential nutrients for bone health. Consuming foods high in magnesium, potassium, and other minerals is beneficial. - Avoiding Harmful Habits
Quitting smoking and moderating alcohol intake are important lifestyle changes that can positively impact bone health. - Bioidentical Hormone Therapy
Some women explore bioidentical hormone therapy as an alternative to conventional hormone replacement therapy (HRT). Pharmaceutical companies synthesize bioidentical hormones to be chemically identical to those naturally produced in the body. However, their safety and efficacy are still under investigation.
It’s crucial to emphasize that alternative treatments are not substitutes for evidence-based medical interventions. Always consult with a healthcare professional before incorporating them, as they may interact with medications or have varying effects on individual health.
Conclusion
In conclusion, early intervention and a comprehensive approach are key to the effective treatment of premenopausal osteoporosis. By understanding the condition, adopting healthy lifestyle changes, and exploring various treatment options, individuals can nurture their bone health and lead fulfilling lives.
If you are facing menopause related issues, menopause treatment at HerMantra can help. Book your free trial online menopause treatment session now.