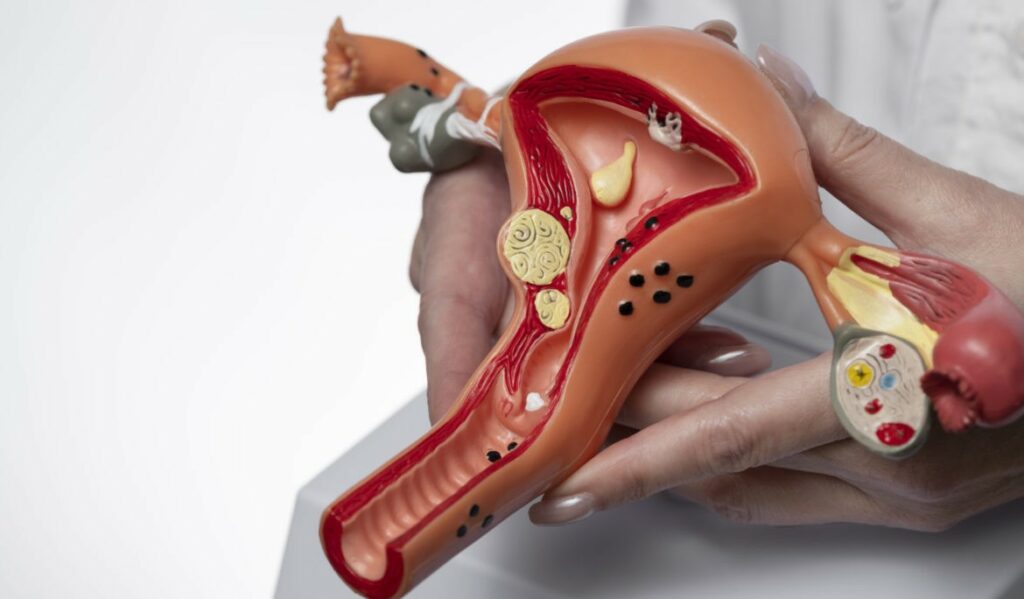
As women transition into menopause, they may assume that concerns related to reproductive health, such as uterine fibroids, are left behind. However, for some, the presence of uterine fibroids can persist and even pose unique challenges. In this blog, we will explore the various treatments for uterine fibroids after menopause, empowering women with the knowledge to make informed decisions about their health and well-being.
Contents
Should Fibroids Be Removed After Menopause?
 The decision to remove fibroids after menopause is not a one-size-fits-all approach and should be carefully considered based on individual circumstances. While it is true that estrogen, a hormone that tends to fuel the growth of fibroids, decreases significantly after menopause, fibroids can persist and cause symptoms in some women. If the fibroids are causing discomfort or affecting the quality of life, removal might be a reasonable option.
The decision to remove fibroids after menopause is not a one-size-fits-all approach and should be carefully considered based on individual circumstances. While it is true that estrogen, a hormone that tends to fuel the growth of fibroids, decreases significantly after menopause, fibroids can persist and cause symptoms in some women. If the fibroids are causing discomfort or affecting the quality of life, removal might be a reasonable option.
However, it’s crucial to weigh the potential benefits against the risks associated with the chosen treatment. Especially considering the overall health and medical history of the individual. In some cases, fibroids after menopause may not cause significant issues. Thus, a watchful waiting approach may be appropriate.
Regular monitoring and discussions with a healthcare provider are essential to evaluate any changes in symptoms and assess the need for intervention. Ultimately, the decision to remove fibroids after menopause should be a collaborative effort between the individual and their healthcare team.
What Are The Some Treatments For Uterine Fibroids After Menopause?
Several treatments for uterine fibroids after menopause are available, depending on the severity of symptoms, individual health considerations, and the woman’s preferences. Here are some common treatments:
Watchful Waiting
Watchful waiting is a strategy often employed when fibroids are small, asymptomatic, or not causing significant discomfort. In postmenopausal women, especially those with fibroids that have not exhibited substantial growth or troublesome symptoms, healthcare providers may opt for a watchful waiting approach. Regular monitoring through pelvic exams, ultrasounds, or other imaging techniques helps track any changes in the size or behavior of the fibroids. This approach acknowledges that, in some cases, fibroids may naturally shrink or become less problematic over time without the need for active intervention.
Hormone Replacement Therapy (HRT)
Hormone Replacement Therapy (HRT) is commonly used to alleviate menopausal symptoms by supplementing declining estrogen levels. However, the use of estrogen in HRT may stimulate the growth of fibroids in some women. For those with both menopausal symptoms and uterine fibroids, healthcare providers carefully weigh the benefits of HRT against the potential risks related to fibroid growth. Individual health history, the severity of menopausal symptoms, and the presence of fibroid-related issues all play a role in determining whether HRT is a suitable option.
Non-Invasive Medical Management
Non-invasive medical management involves the use of hormonal medications, such as gonadotropin-releasing hormone (GnRH) agonists, to induce a temporary menopausal state. This state can lead to a reduction in the size of fibroids and relief from associated symptoms. These medications are typically prescribed for short-term use due to their potential impact on bone density. Non-invasive approaches are favored when preserving fertility or avoiding surgery is a priority.
Minimally Invasive Procedures
Minimally invasive procedures offer alternatives to traditional surgery for women with symptomatic fibroids. Uterine artery embolization (UAE) involves blocking the blood supply to the fibroids, causing them to shrink. Radiofrequency ablation employs targeted heat to destroy fibroid tissue. Both techniques aim to provide symptom relief without the need for major surgery. While these procedures are generally well-tolerated, their suitability depends on factors such as the size, number, and location of fibroids.
Surgical Interventions
Surgical interventions become considerations when fibroids are causing severe symptoms, impacting the quality of life, or if there are concerns about underlying health issues. Myomectomy involves the removal of fibroids while preserving the uterus, which can be relevant for those who wish to maintain fertility. Hysterectomy, on the other hand, entails the removal of the entire uterus and is considered a definitive solution. The decision to undergo surgery depends on factors such as the size and location of fibroids, overall health, and personal preferences.
Ultimately, the choice of treatment for uterine fibroids after menopause should be personalized based on the specific circumstances and preferences of the individual. And it requires thorough discussions with healthcare providers to determine the most suitable approach.
What Are Some Natural Approaches?
 While natural approaches may not guarantee the complete elimination of fibroids, some individuals find relief from symptoms through lifestyle changes and complementary therapies. It’s important to note that scientific evidence supporting the efficacy of these approaches varies, and their effectiveness can vary from person to person. Here are some natural approaches that some individuals consider for managing fibroid symptoms:
While natural approaches may not guarantee the complete elimination of fibroids, some individuals find relief from symptoms through lifestyle changes and complementary therapies. It’s important to note that scientific evidence supporting the efficacy of these approaches varies, and their effectiveness can vary from person to person. Here are some natural approaches that some individuals consider for managing fibroid symptoms:
Dietary Changes
Incorporating dietary changes is a common natural approach to managing fibroid symptoms. An anti-inflammatory diet, which emphasizes whole foods like fruits, vegetables, whole grains, and lean proteins, is often recommended. Foods rich in anti-inflammatory properties, such as fatty fish containing omega-3 fatty acids, turmeric, and ginger, are believed to contribute to reducing inflammation and hormonal imbalances. Additionally, maintaining a diet high in fiber from fruits, vegetables, and whole grains may support overall health and hormonal balance.
Herbal Remedies
Some individuals explore herbal supplements as part of their strategy for managing fibroids. Chasteberry (Vitex), green tea extract, and milk thistle are among the herbs that are thought to have potential benefits for hormonal balance and uterine health. However, it’s crucial to approach herbal remedies with caution, as scientific evidence supporting their effectiveness for fibroid management is limited.
Lifestyle Modifications
Engaging in regular physical activity is not only essential for overall health but may also help manage fibroid symptoms. Exercise contributes to hormonal balance and reduces inflammation, potentially alleviating symptoms such as pelvic pain and discomfort. Weight management is another critical aspect, as obesity has been associated with an increased risk of fibroids. Maintaining a healthy weight through a combination of a balanced diet and regular exercise is encouraged for those seeking natural approaches to fibroid management.
Stress Reduction Techniques
Stress reduction techniques, including yoga and meditation, are recognized for their potential to positively impact hormonal balance and overall well-being. Chronic stress can contribute to hormonal imbalances, potentially exacerbating fibroid symptoms. Incorporating relaxation practices into daily life may help manage stress levels. And, providing relief from symptoms and promoting a sense of overall calm and well-being.
Acupuncture
Acupuncture is a traditional Chinese medicine practice involving the insertion of thin needles into specific points on the body. It is explored by some individuals as a complementary therapy for fibroid symptoms. While research on the effectiveness of acupuncture for fibroids is ongoing and results are varied, some individuals report subjective improvements in symptoms. Acupuncture is generally considered safe when performed by a trained practitioner. However, it’s important to consult with healthcare providers before pursuing this approach.
Limiting Exposure to Environmental Estrogens
 Environmental estrogens, found in plastics, pesticides, and certain household products, can act as endocrine disruptors, potentially influencing hormonal balance. Limiting exposure to these substances is considered a preventive measure for fibroid management. Choosing BPA-free products, opting for organic produce to reduce pesticide exposure, and being mindful of the chemicals present in household items are steps individuals may take. This further helps to minimize their exposure to environmental estrogens and supports overall hormonal health.
Environmental estrogens, found in plastics, pesticides, and certain household products, can act as endocrine disruptors, potentially influencing hormonal balance. Limiting exposure to these substances is considered a preventive measure for fibroid management. Choosing BPA-free products, opting for organic produce to reduce pesticide exposure, and being mindful of the chemicals present in household items are steps individuals may take. This further helps to minimize their exposure to environmental estrogens and supports overall hormonal health.
In all cases, it’s crucial to approach natural approaches with a well-informed perspective and in consultation with healthcare professionals. Regular monitoring and open communication with healthcare providers ensure that chosen strategies align with individual health needs. Thus, contributes to overall well-being.
Conclusion
In conclusion, treatments for uterine fibroids after menopause involve a thoughtful and individualized approach. From watchful waiting and hormonal therapies to minimally invasive procedures and lifestyle changes, there are various options available. Natural approaches like dietary changes, herbal remedies, and stress reduction techniques may offer additional support. However, it’s essential to consult with healthcare professionals. Because they help to determine the most suitable course of action based on individual circumstances.
The key is empowerment through knowledge, fostering open communication with healthcare providers, and making informed decisions that prioritize overall well-being. Each woman’s journey with uterine fibroids after menopause is unique. So, with the right guidance, she can navigate the path that best aligns with her health goals and preferences. If you are facing menopause-related issues, menopause treatment at HerMantra can help. Book your free trial online menopause treatment session now.