Polycystic Ovary Syndrome (PCOS) is a complex endocrine disorder that affects individuals assigned to females at birth. Traditionally associated with reproductive issues such as irregular menstrual cycles and ovarian cysts, PCOS has been the subject of extensive research. However, a lesser-known variant, termed “Adrenal PCOS,” has gained attention in recent years. This variant highlights the interplay between adrenal health and the manifestation of PCOS symptoms, presenting a unique set of challenges for diagnosis and management. In this blog, we have provided detailed information about Adrenal PCOS including its signs, causes and treatment options.
Contents
Understanding PCOS
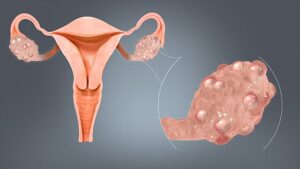
Before delving into Adrenal PCOS, it’s crucial to comprehend the fundamentals of PCOS. PCOS is characterized by hormonal imbalances, insulin resistance, and ovarian dysfunction. Common symptoms include irregular periods, anovulation, and the development of cysts on the ovaries. While the exact cause remains elusive, both genetic and environmental factors contribute to its development.
Adrenal PCOS: Unraveling the Connection
Adrenal PCOS represents a subset of PCOS cases where adrenal glands play a significant role in hormonal dysregulation. The adrenal glands, located on top of the kidneys, are responsible for producing essential hormones, including cortisol and DHEA-S (dehydroepiandrosterone sulfate). These hormones influence various bodily functions, including metabolism, immune response, and the regulation of androgens (male hormones).
In Adrenal PCOS, an overactive adrenal gland produces excessive androgens, contributing to the hormonal imbalances characteristic of PCOS. Elevated levels of androgens, such as testosterone, can disrupt the delicate hormonal equilibrium, leading to the manifestation of PCOS symptoms.
Signs and Symptoms of Adrenal PCOS

Adrenal PCOS, a variant of Polycystic Ovary Syndrome (PCOS), means by the influence of adrenal glands on hormonal imbalances. While some symptoms overlap with classic PCOS, Adrenal PCOS presents unique signs related to adrenal dysfunction. Here are the signs and symptoms commonly associated with Adrenal PCOS:
- Irregular Menstrual Cycles: Adrenal PCOS often manifests as irregular periods, similar to classic PCOS. Menstrual irregularities may include unpredictable cycles, prolonged periods, or even amenorrhea (absence of menstruation).
- Hirsutism (Excessive Hair Growth): Elevated levels of androgens, particularly testosterone, can lead to increased hair growth in areas where males typically grow hair. This may include the face, chest, back, and other traditionally male-patterned areas.
- Acne and Oily Skin: Androgens influence sebum production in the skin, and elevated levels can result in excessive oil production. This may contribute to acne, particularly on the face, chest, and back.
- Scalp Hair Thinning or Loss: Androgen excess in Adrenal PCOS can affect the hair follicles on the scalp, leading to thinning hair or even male-patterned baldness.
- Elevated Androgen Levels: Laboratory tests may reveal elevated levels of androgens such as testosterone. This hormonal imbalance contributes to the physical manifestations of Adrenal PCOS.
- Insulin Resistance: Adrenal PCOS, like classic PCOS, is often associated with insulin resistance. Insulin resistance can lead to elevated blood sugar levels, weight gain, and an increased risk of developing type 2 diabetes.
- Fatigue and Exhaustion: Adrenal glands play a crucial role in regulating cortisol, the body’s primary stress hormone. Adrenal dysfunction in PCOS can lead to chronic stress and fatigue.
- Difficulty Managing Stress: Individuals with Adrenal PCOS may find it challenging to manage stress effectively. Stress can exacerbate hormonal imbalances and worsen symptoms.
- High DHEA-S Levels: Dehydroepiandrosterone sulfate (DHEA-S) is a hormone produced by the adrenal glands. Elevated levels of DHEA-S may be observed in individuals with Adrenal PCOS.
- Weight Management Challenges: Adrenal PCOS may be associated with difficulties in managing weight, with a tendency towards abdominal obesity. Insulin resistance and hormonal imbalances contribute to weight-related challenges.
- Pelvic Pain: Some individuals with Adrenal PCOS may experience pelvic pain or discomfort, similar to classic PCOS, due to ovarian cysts.
It’s essential to note that the symptoms of Adrenal PCOS can vary among individuals, and not everyone with this variant will experience all of these signs.
Causes of Adrenal PCOS

The causes of Adrenal PCOS are rooted in the dysregulation of adrenal gland function and the subsequent impact on hormonal balance. While the precise etiology of Adrenal PCOS is not fully understood, several factors contribute to the development of this variant of Polycystic Ovary Syndrome (PCOS). Here are some potential causes and contributing factors:
- Adrenal Gland Dysfunction: The primary factor in Adrenal PCOS is dysfunction of the adrenal glands, which are responsible for producing hormones such as cortisol and dehydroepiandrosterone sulfate (DHEA-S). Overactivity of the adrenal glands can result in excessive production of androgens, contributing to the hormonal imbalance seen in Adrenal PCOS.
- Chronic Stress: Chronic stress is a significant contributor to Adrenal PCOS. The adrenal glands respond to stress by releasing cortisol, the body’s primary stress hormone. Prolonged periods of stress can lead to adrenal fatigue or dysfunction, impacting cortisol production and, subsequently, hormonal balance.
- Genetic Predisposition: There may be a genetic component to Adrenal PCOS, as with classic PCOS. Individuals with a family history of PCOS or hormonal imbalances may have a higher risk of developing Adrenal PCOS.
- Inflammation: Chronic inflammation can disrupt the normal functioning of the adrenal glands and contribute to hormonal imbalances. Inflammation may be influenced by factors such as diet, lifestyle, and environmental exposures.
- Insulin Resistance: Insulin resistance, a common feature in both classic PCOS and Adrenal PCOS, can contribute to hormonal dysregulation. Insulin resistance leads to increased insulin levels, which, in turn, stimulate the ovaries and adrenal glands to produce more androgens.
- Lifestyle Factors: Unhealthy lifestyle habits, including poor diet, lack of exercise, and inadequate sleep, can contribute to adrenal dysfunction and exacerbate symptoms of Adrenal PCOS.
- Hormonal Imbalances: Imbalances in the delicate interplay of hormones, including cortisol, DHEA-S, and androgens, contribute to the development of Adrenal PCOS. Disruptions in these hormonal pathways can lead to the characteristic symptoms of the condition.
- Environmental Factors: Exposure to endocrine-disrupting chemicals in the environment may play a role in the development of Adrenal PCOS. These chemicals can interfere with the normal functioning of the endocrine system, including the adrenal glands.
- Thyroid Dysfunction: Thyroid disorders, such as hypothyroidism, can influence adrenal function and contribute to hormonal imbalances. The thyroid and adrenal glands are interconnected in the endocrine system.
It’s important to note that Adrenal PCOS likely involves a combination of these factors, and the specific causative factors may vary among individuals.
Impacts of Adrenal PCOS on Women’s Health
The hormonal imbalances associated with Adrenal PCOS can affect various physiological processes, leading to a range of health implications. Here are some of the key impacts of Adrenal PCOS on women’s health:
- Menstrual Irregularities: Adrenal PCOS often results in irregular menstrual cycles, with variations in cycle length and the absence of ovulation. This can lead to challenges in predicting fertility, difficulties in conception, and an increased risk of endometrial issues.
- Fertility Challenges: Irregular ovulation and hormonal imbalances in Adrenal PCOS can contribute to fertility challenges. Women with Adrenal PCOS may experience difficulties in conceiving and may require specialized fertility treatments.
- Hormonal Imbalances: Elevated levels of androgens, such as testosterone, can lead to the development of hirsutism (excessive hair growth), acne, and scalp hair thinning or loss. These manifestations can impact a woman’s self-esteem and quality of life.
- Insulin Resistance and Metabolic Complications: Adrenal PCOS is often associated with insulin resistance, contributing to elevated blood sugar levels. This can lead to an increased risk of developing type 2 diabetes and metabolic syndrome. Managing insulin resistance becomes crucial in preventing long-term metabolic complications.
- Cardiovascular Health Risks: Insulin resistance and metabolic disturbances associated with Adrenal PCOS may elevate the risk of cardiovascular diseases, including hypertension and dyslipidemia. Regular monitoring and lifestyle modifications are essential to mitigate these risks.
- Weight Management Challenges: Women with Adrenal PCOS may find it challenging to manage weight due to insulin resistance and hormonal imbalances. Obesity, particularly central obesity, is a common concern and can exacerbate other health issues.
- Psychological and Emotional Impact: Dealing with the physical symptoms of Adrenal PCOS, such as hirsutism and acne, along with the emotional toll of fertility challenges, can contribute to psychological distress, anxiety, and depression.
- Adrenal Fatigue: Chronic stress and adrenal dysfunction can lead to adrenal fatigue, characterized by persistent fatigue, disrupted sleep patterns, and difficulty coping with stress. Adrenal fatigue can exacerbate existing symptoms and impact daily functioning.
Treatment Options for Adrenal PCOS

The management of Adrenal PCOS involves a comprehensive approach that addresses both adrenal gland dysfunction and the associated hormonal imbalances. Treatment strategies aim to alleviate symptoms, regulate menstrual cycles, and improve overall health. Here are common treatment options for Adrenal PCOS:
Lifestyle Modifications:
- Diet: Adopting a balanced and nutrient-dense diet can help regulate blood sugar levels and manage insulin resistance. Emphasizing whole foods, fiber, and lean proteins while limiting processed sugars and refined carbohydrates is beneficial.
- Exercise: Regular physical activity supports weight management, improves insulin sensitivity, and positively influences hormonal balance. Both aerobic exercise and strength training are valuable components of a comprehensive fitness plan.
Stress Management:
- Mindfulness and Relaxation Techniques: Stress reduction techniques, such as mindfulness meditation, deep breathing exercises, and yoga, can help manage cortisol levels and alleviate the impact of chronic stress on adrenal function.
Hormonal Therapy:
- Oral Contraceptives: Birth control pills containing estrogen and progestin can regulate menstrual cycles, reduce androgen levels, and improve symptoms like acne and hirsutism.
- Anti-Androgen Medications: Medications such as spironolactone may be prescribed to block the effects of androgens and improve symptoms like hirsutism and acne.
Insulin-Sensitizing Medications:
- Metformin: This medication helps to improve insulin sensitivity and manage insulin resistance. It helps to regulate menstrual cycles and reduce the risk of type 2 diabetes.
Fertility Treatments:
- Ovulation Induction: For women experiencing fertility challenges due to irregular ovulation, medications such as clomiphene citrate or letrozole may be prescribed to stimulate ovulation.
- In Vitro Fertilization (IVF): In more severe cases of infertility, assisted reproductive technologies like IVF may be considered.
Thyroid Management:
- Thyroid Medications: If thyroid dysfunction is present, medications such as levothyroxine help to regulate thyroid hormone levels.
Nutritional Supplements:
- Inositol: Inositol, particularly myo-inositol, and D-chiro-inositol, has shown promise in improving insulin sensitivity and menstrual regularity in women with PCOS.
- Vitamin D: Supplementation with vitamin D may be recommended, as deficiencies are common in individuals with PCOS and may impact hormonal balance.
Conclusion
In conclusion, Adrenal PCOS presents a distinctive challenge in the realm of women’s health, emphasizing the critical role of adrenal gland function in hormonal imbalances. A multifaceted approach encompassing lifestyle modifications, hormonal therapies, and stress management is pivotal in mitigating symptoms and improving overall well-being.
As research continues to unveil the intricacies of Adrenal PCOS, collaborative efforts between healthcare providers and individuals will be essential in refining treatment strategies and offering hope for enhanced quality of life for those navigating this complex endocrine disorder. If you are facing PCOS-related issues, PCOS treatment at HerMantra can help. Book your free trial online Pcos treatment session now.



