Polycystic Ovary Syndrome (PCOS) is a common condition affecting women, impacting not only their overall health but also their fertility. In this comprehensive guide, we’ll delve into the complexities of PCOS and its intricate relationship with fertility. From understanding the syndrome to exploring medical interventions and lifestyle adjustments, this article aims to provide insights and support for those navigating the challenging journey of PCOS-related fertility issues.
Contents
Understanding PCOS
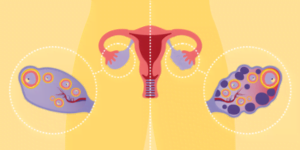
PCOS is a complex hormonal disorder that often involves an imbalance in insulin levels, leading to increased androgen production. The resulting hormonal irregularities can disrupt the normal functioning of the ovaries, affecting the release of eggs during the menstrual cycle.
Identifying PCOS involves recognizing a combination of symptoms such as irregular periods, acne, hair thinning, and weight fluctuations. These indicators, when present, warrant further investigation to assess their impact on fertility.
Link Between PCOS and Fertility
Polycystic Ovary Syndrome (PCOS) is a complex hormonal disorder that intricately intertwines with fertility. Understanding this link is pivotal for individuals and couples grappling with the challenges of PCOS-related fertility issues.
Impact on Ovulation
A cornerstone in the connection between PCOS and fertility lies in its profound impact on ovulation. Ovulation, the release of an egg from the ovaries, is a critical process for conception. In individuals with PCOS, hormonal imbalances, particularly elevated levels of androgens, disrupt the regularity of ovulation. This irregularity significantly reduces the chances of conceiving, creating a major hurdle for couples trying to start a family.
Hormonal Imbalances and Their Role
The hormonal imbalances associated with PCOS play a multifaceted role in influencing fertility. Elevated levels of androgens, including testosterone, not only hinder ovulation but also affect the quality of eggs released during the process. This compromised quality can make it challenging for fertilization to occur successfully. Moreover, these hormonal fluctuations create an unfavorable reproductive environment, further diminishing the likelihood of conception.
Menstrual Irregularities
PCOS often manifests in irregular menstrual cycles, adding another layer to the complexity of its link with fertility. Irregular periods can make it difficult to predict the fertile window, hindering natural conception efforts. Understanding and addressing these menstrual irregularities are crucial steps in navigating the path to fertility for individuals with PCOS.
Insulin Resistance
Another significant aspect of the PCOS-fertility link is insulin resistance. Many individuals with PCOS exhibit resistance to insulin, a hormone that regulates blood sugar. Insulin resistance can lead to increased production of insulin, which, in turn, contributes to elevated androgen levels. This intricate interplay of hormones further disrupts the delicate balance required for optimal fertility.
Inflammation and Oxidative Stress
PCOS is often associated with chronic low-grade inflammation and oxidative stress. These conditions can negatively impact the reproductive system, affecting the health of eggs and the lining of the uterus. Addressing inflammation and oxidative stress becomes paramount in enhancing fertility outcomes for individuals with PCOS.
Diagnosing PCOS and Fertility Issues

Accurate diagnosis is a fundamental step in understanding and addressing the intricate relationship between Polycystic Ovary Syndrome (PCOS) and fertility. Medical professionals employ a variety of tests and examinations to assess the presence of PCOS and identify specific challenges related to conception.
Medical Tests and Examinations
- Hormone Level Assessments: Blood tests are crucial for evaluating hormone levels, including androgens such as testosterone. Elevated androgen levels are a key indicator of PCOS and can provide insights into its impact on fertility.
- Insulin Resistance Testing: Given the association between PCOS and insulin resistance, tests measuring insulin levels and glucose tolerance help identify potential metabolic factors affecting fertility.
- Ultrasound Imaging: Transvaginal ultrasound is commonly used to visualize the ovaries. The presence of small cysts (follicles) on the ovaries, a characteristic feature of PCOS, can be observed through this imaging technique.
- Menstrual History Review: A thorough review of menstrual history is essential. Irregular periods or prolonged cycles can be indicative of hormonal imbalances associated with PCOS, impacting ovulation and fertility.
Fertility Assessments
- Ovulation Monitoring: Tracking ovulation through methods like basal body temperature charting or ovulation predictor kits provides valuable information about the regularity of ovulation.
- Semen Analysis for Partners: Since fertility is a shared responsibility, assessing the male partner’s semen quality is vital. Semen analysis helps identify any male factor infertility issues that may coexist with PCOS-related fertility challenges.
- Hysterosalpingography (HSG): This test evaluates the condition of the fallopian tubes and the uterus. It can identify potential blockages or abnormalities that might affect fertility.
- Endometrial Biopsy: In some cases, an endometrial biopsy may be recommended to assess the health of the uterine lining, ensuring it is conducive to implantation.
Medical Treatments for PCOS and Fertility
Addressing fertility challenges associated with Polycystic Ovary Syndrome (PCOS) often involves medical interventions aimed at regulating ovulation, managing hormonal imbalances, and optimizing the overall reproductive environment. Here, we’ll explore some common medical treatments employed to enhance fertility in individuals with PCOS.
Medications for Inducing Ovulation
- Clomiphene Citrate (Clomid): This oral medication is a first-line treatment for inducing ovulation. It works by stimulating the release of hormones necessary for ovulation, promoting regular menstrual cycles, and improving the chances of conception.
- Letrozole (Femara): Another medication used to induce ovulation, Letrozole is often considered when Clomiphene Citrate is not effective or well-tolerated. It helps regulate the menstrual cycle and enhance fertility.
- Gonadotropins: Injectable hormones, such as follicle-stimulating hormone (FSH) and luteinizing hormone (LH), may be prescribed to stimulate the ovaries directly. This approach is often considered when oral medications are ineffective.
In Vitro Fertilization (IVF)
- Ovulation Induction in IVF: In IVF, medications are used to stimulate the ovaries to produce multiple eggs. This is followed by the retrieval of mature eggs, which are then fertilized in a laboratory setting. The resulting embryos are subsequently transferred to the uterus.
- Intracytoplasmic Sperm Injection (ICSI): ICSI may be incorporated into the IVF process, especially if there are male-factor infertility issues. This technique involves the direct injection of a single sperm into an egg, increasing the likelihood of successful fertilization.
Natural Approaches to Enhance Fertility
In conjunction with medical interventions, incorporating natural approaches can further support fertility goals for individuals with PCOS.
Herbal Remedies and Supplements
Certain herbs and supplements, such as myo-inositol and vitamin D, have shown promise in managing PCOS symptoms and enhancing fertility. However, it’s crucial to consult with healthcare professionals before incorporating these into one’s routine.
Emotional and Psychological Aspects
Dealing with fertility challenges can take a toll on emotional well-being. Recognizing and addressing the emotional and psychological aspects of PCOS-related fertility struggles is essential for holistic care.
Coping with the Emotional Toll of Fertility Struggles
The emotional impact of infertility can be overwhelming. Seeking support from loved ones, joining support groups, or engaging in counseling can help individuals and couples navigate these challenges.
Lifestyle and Dietary Factors
Maintaining a healthy lifestyle is key to managing PCOS and promoting fertility. Regular exercise, stress management, and adequate sleep contribute to overall well-being and can positively impact reproductive health.
Diet plays a crucial role in managing PCOS symptoms. A balanced and nutrient-rich diet, focused on controlling insulin levels, can support hormonal balance and enhance fertility.
Tips for Couples Dealing with PCOS and Fertility
Here are some practical tips to help couples facing PCOS-related fertility challenges enhance their chances of conception and maintain emotional well-being:
Communication and Mutual Support
- Open and Honest Communication: Foster a climate of open communication. Discuss feelings, concerns, and expectations regarding fertility, ensuring both partners feel heard and understood.
- Educate Each Other: Take the time to learn about PCOS together. Understanding the condition and its impact on fertility can create a shared knowledge base, fostering a stronger sense of unity.
- Set Realistic Goals: Establish realistic and achievable fertility goals. Recognize that the journey may involve a combination of medical interventions, lifestyle changes, and emotional support.
Seeking Professional Help When Needed
- Consult with Fertility Specialists: Timely consultation with fertility specialists is crucial. Seek professional guidance to understand the specific fertility challenges associated with PCOS and explore suitable treatment options.
- Attend Appointments Together: Whenever possible, attend medical appointments together. This collaborative approach ensures both partners are actively involved in the decision-making process.
Emotional Support
- Lean on Each Other: Emotional support is paramount. Be there for each other during both highs and lows. The emotional toll of fertility challenges can be eased through shared experiences and mutual understanding.
- Consider Counseling: Professional counseling can provide valuable tools for coping with the emotional aspects of fertility struggles. Individual and couples counseling sessions offer a safe space to explore emotions and develop coping strategies.
Preventive Measures for PCOS-Related Fertility Issues
Here are some preventive measures for PCOS-related fertility issues:
- Quit Smoking and Limit Alcohol Intake: Smoking and excessive alcohol intake can negatively impact fertility. Quitting smoking and moderating alcohol consumption can improve overall health and fertility outcomes.
- Manage Stress: Chronic stress can exacerbate hormonal imbalances. Practice stress-reducing techniques such as yoga, meditation, deep breathing, or mindfulness to promote emotional well-being.
- Manage Insulin Resistance: Since insulin resistance is common in PCOS, managing blood sugar levels is crucial. Focus on a low-glycemic diet, which can help stabilize blood sugar levels. Some women with PCOS may benefit from medications that improve insulin sensitivity, as prescribed by a healthcare provider.
- Regular Monitoring and Medical Check-ups: Regularly monitor your menstrual cycles and seek medical advice if you notice irregularities. Early detection and management of PCOS-related issues can help prevent complications.
Conclusion
In conclusion, understanding the dynamics of PCOS and its impact on fertility is the first step toward finding effective solutions. Whether through lifestyle adjustments, medical interventions, or a combination of both, there is hope for individuals with PCOS to achieve their dreams of parenthood. By staying informed, seeking support, and embracing a proactive approach, the journey to conception can become more manageable.
If you are facing PCOS related issues, pcos treatment at HerMantra can help. Book your free trial online pcos treatment session now.



