PCOS, a common hormonal disorder, often presents obstacles to natural conception due to irregular ovulation. However, with advancements in reproductive medicine, ovulation induction has emerged as a promising solution for those navigating fertility challenges associated with PCOS. In this comprehensive guide, we will delve into the intricacies of ovulation induction in PCOS, exploring the science behind it, and empowering individuals with the knowledge needed to take charge of their fertility journey.
Contents
Does Ovulation Induction Work With PCOS?
 Ovulation induction has shown promising results in addressing fertility challenges associated with Polycystic Ovary Syndrome (PCOS). Women with PCOS often experience irregular menstrual cycles and anovulation (lack of ovulation), which can significantly hinder natural conception. Ovulation induction involves using medications to stimulate the ovaries, regulate the release of eggs, and increase the chances of successful ovulation.
Ovulation induction has shown promising results in addressing fertility challenges associated with Polycystic Ovary Syndrome (PCOS). Women with PCOS often experience irregular menstrual cycles and anovulation (lack of ovulation), which can significantly hinder natural conception. Ovulation induction involves using medications to stimulate the ovaries, regulate the release of eggs, and increase the chances of successful ovulation.
By carefully monitoring the ovarian response through ultrasound and hormonal assessments, healthcare providers can tailor treatment plans to optimize the chances of conception in women with PCOS. While ovulation induction in PCOS has proven effective for many individuals, success rates can vary based on factors.
It’s essential for individuals undergoing ovulation induction to work closely with their healthcare team to ensure personalized treatment plans and ongoing monitoring. Moreover, lifestyle modifications are often recommended alongside medical interventions to enhance the overall success of ovulation induction in PCOS.
What Is The Importance Of Ovulation Induction?
Ovulation induction holds significant importance, particularly for individuals facing challenges with fertility, and it plays a crucial role in assisted reproductive technologies. Here are several key aspects highlighting the importance of ovulation induction:
- Enhances Fertility Treatment Options
For couples undergoing fertility treatments, ovulation induction is a foundational step. It allows healthcare providers to better control and optimize the timing of ovulation, increasing the chances of successful fertilization during natural conception or procedures like intrauterine insemination (IUI) and in vitro fertilization (IVF).
- Improves Timing for Conception
Ovulation induction helps pinpoint the optimal time for conception. By closely monitoring the development of ovarian follicles through ultrasound and hormonal assessments, healthcare providers can determine when the eggs are mature and ready for release.
- Addresses Unexplained Infertility
In cases of unexplained infertility, where no specific cause has been identified, ovulation induction provides a targeted approach to addressing potential ovulatory dysfunction. By stimulating ovulation, this intervention aims to overcome one of the common barriers to conception, offering a more focused treatment strategy.
- Minimizes Time to Conception
Ovulation induction can significantly reduce the time it takes for couples to conceive, especially when underlying ovulatory issues are present. By optimizing the natural fertility window or aligning with assisted reproductive technologies, ovulation induction helps couples on their fertility journey achieve pregnancy in a more time-efficient manner.
Overall, ovulation induction plays a pivotal role in addressing various fertility challenges, providing a targeted and effective means to regulate ovulation. Ultimately, enhances fertility treatments, and increases the chances of successful conception for individuals and couples struggling to achieve pregnancy.
What Are Some Strategies Used In Ovulation Induction In PCOS?
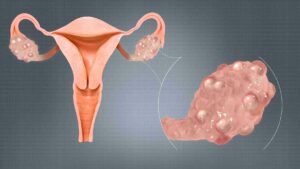 Ovulation induction in PCOS involves various strategies aimed at regulating the menstrual cycle and promoting the release of eggs. Here are some common strategies used in ovulation induction for PCOS:
Ovulation induction in PCOS involves various strategies aimed at regulating the menstrual cycle and promoting the release of eggs. Here are some common strategies used in ovulation induction for PCOS:
Clomiphene Citrate (Clomid)
This is commonly known as Clomid, is an oral medication that serves as a cornerstone in ovulation induction for women with PCOS. It operates by blocking estrogen receptors in the brain, leading to an increase in the production of follicle-stimulating hormone (FSH) and luteinizing hormone (LH). This heightened hormonal activity prompts the ovaries to develop and release mature eggs. Typically prescribed for a specific period in the menstrual cycle, Clomid is regularly monitored through ultrasound and hormone level assessments to ensure the optimal dosage and effectiveness.
Letrozole (Femara)
Letrozole is another oral medication commonly used in ovulation induction, offering an alternative for individuals who may not respond well to Clomid. Unlike Clomid, which blocks estrogen receptors, letrozole works by inhibiting the production of estrogen itself. By doing so, it indirectly stimulates the release of FSH and promotes a more favorable environment for ovulation. Letrozole has demonstrated success in cases where Clomid may have been ineffective or caused undesirable side effects, making it a valuable option for enhancing fertility in women with PCOS.
Gonadotropins (Injectable Fertility Medications)
Injectable gonadotropins represent a more potent form of ovulation induction, often reserved for cases where oral medications prove insufficient. These medications, typically administered through injections, directly supply FSH and LH to stimulate ovarian follicle development. While highly effective, gonadotropin therapy requires careful monitoring due to the increased risk of ovarian hyperstimulation syndrome (OHSS) and multiple pregnancies. Close collaboration between the patient and healthcare team ensures precise dosage adjustments and minimizes potential risks.
Ovulation Monitoring
Ongoing monitoring is a critical component of any ovulation induction strategy. Regular ultrasound scans track the growth of ovarian follicles, providing insights into their maturation. Simultaneously, blood tests measure hormone levels, guiding healthcare providers in assessing the effectiveness of the chosen medication. This dynamic monitoring allows for timely adjustments to medication dosages. Hence, it ensures a balanced and controlled ovarian response.
Trigger Shot (hCG injection)
In certain instances, a trigger shot in the form of a human chorionic gonadotropin (hCG) injection is administered. This injection precisely times the release of mature eggs from the ovarian follicles, optimizing the chances of successful fertilization. The trigger shot is a crucial element in coordinating the final stages of ovulation induction and is administered when ultrasound and hormone assessments indicate that the follicles have reached an optimal size. This precise timing is pivotal for couples aiming to conceive, further illustrating the personalized and strategic nature of ovulation induction procedures.
It’s important to note that the choice of strategy depends on individual factors such as the severity of PCOS, response to previous treatments, and the patient’s overall health. Ongoing communication and collaboration with healthcare providers are essential to tailor the approach to each person’s unique circumstances.
How Can I Induce Ovulation Naturally With PCOS?
 Inducing ovulation naturally with PCOS can be challenging. However, certain lifestyle modifications may help regulate your menstrual cycle and enhance your chances of ovulating. It’s important to note that while these strategies may be beneficial, individual responses can vary, and consulting with a healthcare provider is crucial for personalized guidance. Here are some natural approaches to consider:
Inducing ovulation naturally with PCOS can be challenging. However, certain lifestyle modifications may help regulate your menstrual cycle and enhance your chances of ovulating. It’s important to note that while these strategies may be beneficial, individual responses can vary, and consulting with a healthcare provider is crucial for personalized guidance. Here are some natural approaches to consider:
Maintain a Healthy Diet
Adopting a balanced and nutritious diet is fundamental in managing PCOS and promoting regular ovulation. Focus on whole foods, including fruits, vegetables, lean proteins, and whole grains. Limit refined carbohydrates and sugars, as these can contribute to insulin resistance commonly associated with PCOS. Consider consulting with a nutritionist to create a diet plan tailored to your needs.
Regular Exercise
Engaging in regular physical activity can help improve insulin sensitivity and regulate hormonal balance. Aim for at least 150 minutes of moderate-intensity exercise per week. Activities such as brisk walking, jogging, cycling, or yoga can be beneficial. Exercise not only supports overall health but can also positively impact ovulation in women with PCOS.
Maintain a Healthy Weight
Achieving and maintaining a healthy weight is crucial for managing PCOS symptoms and promoting regular ovulation. Even a modest weight loss of 5-10% of your body weight can have significant benefits. Consult with a healthcare provider or a registered dietitian to develop a realistic and sustainable weight management plan.
Manage Stress
Chronic stress can exacerbate hormonal imbalances and interfere with regular ovulation. Incorporate stress-reducing techniques such as meditation, deep breathing exercises, yoga, or mindfulness into your daily routine. Adequate sleep is also essential for overall hormonal balance and reproductive health.
Herbal Supplements
Some herbal supplements are believed to have potential benefits for women with PCOS. For example, spearmint tea may help reduce androgen levels, and cinnamon might have insulin-sensitizing properties. However, it’s crucial to approach herbal supplements with caution and consult with a healthcare provider before incorporating them into your routine, as they can interact with medications or have contraindications.
Remember that individual responses to these strategies can vary. And what works for one person may not work for another. It’s strongly advisable to consult with a healthcare provider, preferably one with expertise in reproductive endocrinology or fertility, to develop a personalized plan tailored to your specific situation.
Conclusion
In conclusion, understanding and embracing the journey of ovulation induction in PCOS empowers individuals with valuable insights and strategies to navigate fertility challenges. From the science behind medications like Clomid and Letrozole to the personalized nature of treatment plans and the importance of lifestyle modifications, this comprehensive guide sheds light on the multifaceted aspects of promoting ovulation naturally.
Ultimately, this guide serves as a beacon of support, offering hope and practical guidance for individuals and couples aspiring to build their families despite the complexities posed by PCOS. If you are facing PCOS-related issues, PCOS treatment at HerMantra can help. Book your free trial online pcos treatment session now.