Polycystic Ovarian Syndrome (PCOS) is a complex hormonal disorder that can manifest in various ways, affecting not only reproductive health but also skin conditions. One such dermatological concern associated with PCOS is seborrheic dermatitis. In this blog, we will explore the connection between PCOS and seborrheic dermatitis and discuss effective treatment strategies to manage this skin condition.
Contents
What Is Seborrheic Dermatitis?
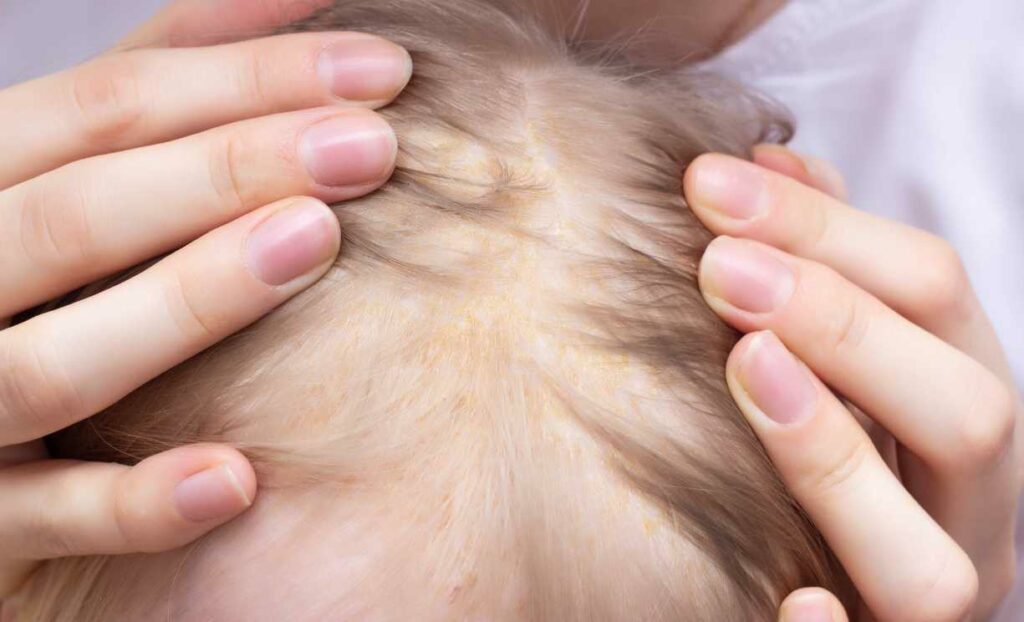
Seborrheic dermatitis is a common skin condition that often appears as red, itchy, and flaky patches on the skin. It can affect various areas, including the scalp, face, and oily regions of the body. The condition is linked to an overgrowth of yeast on the skin and is more likely to occur where there are more oil-producing glands. Seborrheic dermatitis can be chronic, meaning it tends to come and go. While the exact cause is not fully understood, factors such as stress, certain medical conditions, and hormonal changes can contribute to its development. It’s not contagious, and while it can be persistent, effective treatments, including medicated shampoos and creams, can help manage the symptoms and provide relief.
Why does PCOS Cause Seborrheic Dermatitis?
Polycystic Ovarian Syndrome (PCOS) can contribute to the development of seborrheic dermatitis due to hormonal imbalances. In PCOS, there is an increase in male hormones, particularly testosterone. This hormonal shift influences the skin’s sebaceous glands, leading to an overproduction of oil. The excess oil, in turn, creates an environment conducive to the growth of yeast on the skin, which is a key factor in seborrheic dermatitis. Essentially, the hormonal changes in PCOS create conditions where the skin becomes more prone to inflammation, redness, and flakiness characteristic of seborrheic dermatitis. Understanding this link helps in addressing not just the skin symptoms but also the underlying hormonal issues associated with PCOS.
Effective Treatment Options For Seborrheic Dermatitis PCOS
Effective treatment of seborrheic dermatitis in the context of PCOS involves a combination of targeted strategies. Here are some effective treatment approaches:
- Hormonal Management: Addressing the hormonal imbalances associated with PCOS is crucial. Consultation with a healthcare provider can also help explore hormonal therapies or lifestyle changes that regulate androgen levels, potentially reducing the severity of seborrheic dermatitis.
- Medicated Shampoos: For seborrheic dermatitis on the scalp, the use of medicated shampoos containing antifungal agents such as ketoconazole, selenium sulfide, or zinc pyrithione can help control flaking and itching.
- Topical Steroids: In cases of mild to moderate seborrheic dermatitis, topical corticosteroids may be prescribed to reduce inflammation and alleviate symptoms. However, prolonged use should be monitored by healthcare professionals.
- Anti-Inflammatory and Antifungal Creams: Topical creams containing anti-inflammatory agents or antifungal medications can be applied to affected areas on the face or body to reduce redness and control the overgrowth of yeast.
- Gentle Skincare Routine: Adopting a gentle skincare routine is essential. Use mild, fragrance-free cleansers and moisturizers to avoid irritating the skin further.
- Avoiding Triggers: Identify and avoid triggers that may worsen seborrheic dermatitis, such as stress, harsh weather conditions, or certain skincare products.
- Dietary Modifications: While evidence is limited, some individuals may find relief by making dietary changes. Consultation with a nutritionist can help explore potential modifications, such as reducing sugar and processed food intake.
- Stress Management: Stress can exacerbate seborrheic dermatitis symptoms. Adopting stress management techniques, such as mindfulness or yoga, can contribute to overall well-being.
- Regular Follow-ups: Regular consultations with healthcare professionals allow for monitoring the progress of treatment and making adjustments as needed. This ensures a tailored and effective approach.
Medications For Seborrheic Dermatitis
Several medications, both over-the-counter and prescription, can help manage seborrheic dermatitis. The choice of medication depends on the severity of the condition, the areas affected, and individual response. Here are common medications used for seborrheic dermatitis:
- Calcineurin Inhibitors: Topical calcineurin inhibitors like tacrolimus and pimecrolimus may be recommended for areas where corticosteroids are not suitable, such as the face.
- Coal Tar Preparations: Coal tar preparations, available in shampoos, creams, or ointments, can help reduce scaling and inflammation. They are available over the counter and by prescription.
- Prescription-strength Shampoos: In addition to antifungal agents, prescription shampoos may contain other ingredients such as salicylic acid or coal tar to address symptoms on the scalp.
- Oral Antifungal Medications: In severe cases or when other treatments are ineffective, oral antifungal medications such as fluconazole or itraconazole may be prescribed. These are typically reserved for specific situations and are monitored closely due to potential side effects.
- Topical Antibiotics: If there is a bacterial component to the dermatitis, topical antibiotics may help reduce bacterial colonization.
It’s important to use these medications as directed by healthcare professionals, as overuse or misuse can lead to side effects. Additionally, some medications may be more suitable for certain areas of the body, so the choice may vary depending on whether the condition affects the scalp, face, or other body parts.
Lifestyle Changes For Managing Seborrheic Dermatitis
In addition to medical interventions, incorporating certain lifestyle changes can contribute to the effective management of seborrheic dermatitis, particularly in the context of PCOS. Here are lifestyle modifications that may help:
- Maintain a Healthy Diet: Focus on a well-balanced diet rich in fruits, vegetables, lean proteins, and whole grains. While there’s no specific “seborrheic dermatitis diet,” overall nutritional health can support skin function.
- Hygiene Practices: Keep the affected areas clean but avoid excessive washing, as this can strip the skin of natural oils. Use mild, fragrance-free cleansers to avoid irritation.
- Stress Management: Practice stress-reducing techniques such as meditation, deep breathing exercises, or yoga. Stress can exacerbate seborrheic dermatitis symptoms, and managing stress contributes to overall skin health.
- Regular Exercise: Engage in regular physical activity, as exercise promotes circulation and overall well-being. However, avoid excessive sweating, as this can trigger seborrheic dermatitis flare-ups.
- Adequate Sleep: Ensure you get sufficient, quality sleep. Sleep is essential for skin repair and overall health.
- Avoid Triggers: Identify and avoid factors that trigger seborrheic dermatitis flare-ups, such as certain skincare products, extreme weather conditions, or allergens.
- Avoid Harsh Products: Choose skincare and haircare products that are gentle and hypoallergenic. Avoid products with harsh chemicals or fragrances that can irritate the skin.
- Sun Protection: Protect your skin from the sun using sunscreen with a high SPF. Sunburn can worsen seborrheic dermatitis symptoms.
- Humidity Control: In humid conditions, use air conditioning or a dehumidifier to control indoor humidity levels. High humidity can exacerbate seborrheic dermatitis.
- Dietary Considerations: While individual responses vary, some people find relief by limiting foods that may contribute to inflammation, such as processed sugars and dairy. Experiment with dietary changes under the guidance of a healthcare professional.
How Long Does It Take To Treat Seborrheic Dermatitis?
The duration of treatment for seborrheic dermatitis can vary from person to person. In simple terms, it depends on the severity of the condition and how well an individual responds to it. Mild cases may see improvement within a few weeks of consistent treatment, while more severe or chronic cases may require a more extended period.
It’s important to follow the treatment plan and to be patient as the skin heals. Regular follow-ups with a healthcare provider or dermatologist allow for adjustments to the treatment plan based on the individual’s progress, ensuring the most effective and personalized approach to managing seborrheic dermatitis.
Conclusion
In conclusion, addressing seborrheic dermatitis in the context of Polycystic Ovarian Syndrome (PCOS) requires a multifaceted treatment that considers both the skin condition and the underlying hormonal imbalances. The link between PCOS and seborrheic dermatitis is clear, with hormonal fluctuations contributing to the development and exacerbation of skin symptoms. The effective management of seborrheic dermatitis involves a combination of medical interventions, lifestyle modifications, and ongoing care.
It’s essential to work closely with healthcare professionals to tailor a personalized plan that meets specific needs. Regular follow-ups allow for adjustments to the treatment strategy based on the individual’s progress, ensuring optimal results. By addressing both the hormonal aspects of PCOS and the dermatological manifestations of seborrheic dermatitis, individuals can take proactive steps toward healthier skin and overall well-being.